The Bio-Psycho-Social Approach is a comprehensive framework used in psychology and healthcare to understand human behavior and health. It recognizes that people are complex beings, influenced by biological, psychological, and social factors. This approach aims to integrate these three factors to provide a more holistic understanding of individuals and their experiences. By considering the interplay between these factors, the Bio-Psycho-Social Approach offers a more complete understanding of human behavior and health, allowing for more effective interventions and treatments. In this essay, we will explore the key components of the Bio-Psycho-Social Approach and how it incorporates biological, psychological, and social factors in understanding human behavior and health.
The idea that mental states are influenced by many interacting processes, such as bodily processes, personality dispositions and life events, is a very old one. It was well articulated by the early Greek physicians over 2000 years ago and has existed in many cultures old and new Oackson, 1986). Early forerunners of the modern biopsychosocial approach can be found in Meyers’ psychobiology approach (Rutter, 1986), behavioural medicine and psychosomatic medicine (Kiesler, 1999). The biopsychosocial approach, however, is most closely identified with the cardiologist Engel (1977), who in the 1960s used it to understand heart disease. Engel pointed out that heart disease was often the end point of a large variety of cultural, social and psychological factors impinging on the cardiovascular system. These include factors such as genetic vulnerabilities, poverty and diet, smoking and exercise, and coping with stress factors. The pathophysiology of heart disease is real enough, but one will have limited understanding of it and grossly inadequate means of prevention if one does not understand psychosocial interactions with the cardiovascular system. Since then many psychologists have contributed to this approach, and Kiesler (1999) offers an excellent overview of the history of the biopsychosocial approach and its current application to mental health. In its application to mental disorders the biopsychosocial approach is critical of the narrow focus of biomedical approaches. One thing is clear, however: that although many clinicians of all types pay lip service to a biopsychosocial approach, few actually adopt it in their clinical practice or research. The main reasons are that clinicians do not understand it and it calls for radical shifts in research, training and practice (Gilbert, 1995; Kiesler, 1999). Moreover, as Meehl (1995) points out, psychologists are often unaware of psychiatry’s often inappropriate use of its own biomedical model.
The study of interactions
Bio-Psycho-Social Model of Health and Illness Venn Diagram
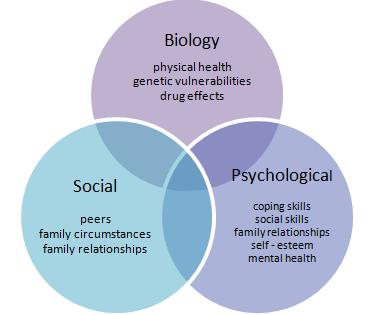
At its best the biopsychosocial approach is holistic but is also more than that. The biopsychosocial approach addresses the complexity of interactions between different domains of functioning and argues that it is the interaction of domains that illuminate important processes. Two examples will be briefly explored here: the physiological effects of social interactions and the importance of individual differences. To take the first example, there is now considerable evidence that, from the day we are born, the quality of our social relationships has a major impact on a host of physiological systems, including cardiovascular, immune and hormonal (Cacioppo, et al., 2000). The way these mature in the contexts of loving, abusive or neglectful environments affects dispositions for affect regulation (Schore, 2001). Indeed, as Schore (2001) outlines, there is a growing literature on the importance of the quality of attachment relationships to brain maturation and that internal working models of attachment (models that can increase vulnerability to later disorders) reflect physiological as well as psychological differences. Negative experiences (for example, parental unresponsiveness, coldness, abuse) are associated with various stress responses (Perry, et al., 1995).
Abused people exhibit increased stress system activation and poorer recovery from stress than non-abused people (Heim, et al., 2000), which has been related to depression vulnerability (Gilbert, 2001; Hart, et al., 1996). Prenatal factors such as maternal stress and drug taking also influence the earliest maturation of fetal physiological systems and can give rise to vulnerabilities (Allen, et al., 1998). Such factors are themselves related to maternal social context and early history. Hence, our whole physical being is therefore an embedded one; we are located in a sea of interactions and values that shape our physical selves. Styles of interaction and social values in turn have histories that transcend individual lives. This shaping can be for good or ill.
Physiology Matters
Clinical psychologists sometimes give the impression that physiological and genetic variation are irrelevant to suffering. The biopsychosocial approach, however, pays due regard to the physiology of mental states, for we are embodied, feeling beings – not just collections of internal schema or behavioural strategies. Moreover, as we understand more about our affect systems and unconscious processing, and how these are involved in experiences of the self, it is becoming increasingly clear that many forms of self-construction are themselves end points of complex social-physiological interactions routed in evolved regulator systems (Panskepp, 1998).
If we focus on depression, it is clear that the physical picture of depression is real enough with abundant evidence of disturbances of physiology (for example, in stress systems and sleep; McGuade and Young, 2000). Depression is a horrible, affect-laden experience that people often feel trapped in. Even for those with (so called) sub-syndromal depressions such as dysthymia, there is good evidence that, as in major depression, there are significant physiological disturbances of functioning (for example, of stress, immune and neurotransmitters systems; Griffiths et al., 2000). New work is exploring the interaction between mood and immune systems (Anisman and Merali, 1999) and the way depression compromises immune functioning, increasing vulnerability to a range of physical disorders (Maes, 1995; Martin, 1997). Even more worrying are the findings that those who are chronically stressed may be vulnerable to subtle forms of brain damage due to the effects of cortisol on neuronal pathways (Sapolsky, 1996; 2000).
However, because depression and anxiety are like many other disorders, which are end states of interacting processes (Akiskal and Mckinney, 1975), we cannot assume that physiological disturbancel tells us much about cause. Indeed, although (for example) genes play a role in some disorders (see for example, Schmidt and Schulkin, 1999), understanding gene transmission is only one of a multitude of factors and pathways that influence how depression and anxiety, in their various physical forms, arise and are passed from generation to generation (for example, via abuse, emotional coldness) or within groups (for example, war, poverty, acceptance of domestic violence, social exclusions). Moreover, social contexts and stress hormones can turn genes on and off; see Ridley (2000) for a fascinating discussion. Many people can become very ill because of toxic environments, and such illnesses are not merely social constructions (although one could argue the whole concept of what constitutes an “illness” is a construction of sorts). There are in fact a host of environmental stressors such as loss of control over adversity, early separation, attachment loss, social support, defeat and social harassment (bullying) that produce profound physiological disturbances and negative states of mind (Gilbert, 2001; Wilkinson, 1996).
So the biopsychosocial approach argues that our physiological systems, including our genes, are not autonomous encapsulated systems. Rather, they can be relatively open and flexible, responding to the demands placed upon them; this is the genotype-phenotype aspect of our functioning. Even for people who hear malevolent voices, the power and dominance of the voices is related to their general perception of how they feel in relation to others in their lives (Birchwood, et 2000). However, as physiological systems become disturbed they will alter psychological and behavioural systems, which may produce further amplifying cycles of dysfunction and painful states of mind and sense of self These feedback systems are themselves complex and involve processes such as activating latent negative self-schema, affect memory (retrieval and encoding), rumination and coping options (Gilbert, 2001).
One might think that the biopsychosocial approach makes good sense, but in fact biopsychosocial approaches are often poorly formulated, poorly taught and rarely adopted (Kiesler, 1999). Within psychiatry the problem has been seen as the consequence of the continuing dominance of Western philosophical notions of dualism, as captured by Eisenberg’s (1986; 2000) critique of “brainless and mindless” science. We, in clinical psychology, are also along way from acknowledging the implications of adopting a genuine biopsychosocial approach (Gilbert, 1995).
Individual Differences
It is clear that there are major individual differences in how people respond to life events and treatment. Disease models always struggle with individual differences and reflect the centuries- long dispute between the Platonic, disease-focused and Hippocratic, person-focused approaches within medicine, and these disputes often get polarized in unhelpful ways (Kendell, 1975). However, because the biopsychosocial approach is inherently interactional it offers away out of these polarities. Not only does it focus on interactions between domains in a wide sense (for ex- ample, on how poverty or lifestyles affect rates of disorders) but also on the need for clinicians to be mindful of interactions within individuals. For genetic, historical or cultural reasons the way your systems interact may be quite different to mine. Even the most basic of differences, for example gender, have been poorly studied and integrated into clinical psychology, despite the growing evidence that men and women may have evolved under different selective pressures and that the triggers of stress and (physiological) responses to stress may differ between them (Taylor et al., 2000). Clearly we need a much more gender sensitive approach to many disorders (Hankin and Abramson, 2001).
Conclusion
For clinical psychology to become a genuinely integrative profession, capable of utilizing scientific findings from a multitude of areas, it is vital we do not confuse the biopsychosocial approach with psychiatry’s use of the biomedical model (Kiesler, 1999; Meehl, 1995). The biopsychosocial approach is ideally suited to cope with the increasing complexities of the clinical sciences, because its focus is on interactions in various domains. The competitive dynamics between professions and between different schools of therapy are understandable as basic human dispositions to assert their views over those of others, but from a scientific and therapeutic point of view this is often unhelpful. We need to break the shackles of brainlessness verses mindlessness, as well as our often decontextualized and desocialized clinical sciences (Eisenberg, 1986; 2000). At the risk of sounding competitive myself, I do believe that clinical psychologists could and should be at the forefront of developing biopsychosocial models of disorders and of interventions. Understanding the interaction between evolved brains, social contexts and experienced selves is the challenge.